Learn how trigger point injections can relieve muscle knots that contribute to joint pain. Discover conditions treated, procedure details, and expected outcomes.
If you suffer from chronic joint pain, you may have noticed that the pain isn’t always confined to the joint itself. Sometimes it radiates to nearby muscles, or you feel knots and tightness that seem to make the joint pain worse.
These knots are called trigger points – hyperirritable spots in skeletal muscle that can cause local and referred pain. They are often overlooked in conventional orthopedics, yet they play a significant role in many chronic pain conditions, including those affecting the shoulders, neck, lower back, hips, and knees.
At Joint Health Solutions, we use trigger point injections (TPIs) as part of our comprehensive, root‑cause approach. TPIs can relax tight muscles, break pain cycles, and improve the effectiveness of other treatments like physical therapy and regenerative medicine.
In this article, we’ll explain what trigger points are, how they contribute to joint pain, and what to expect from trigger point injections.
Trigger points are discrete, focal areas of muscle spasm or tightness. They develop when muscle fibers contract and fail to relax, often due to:
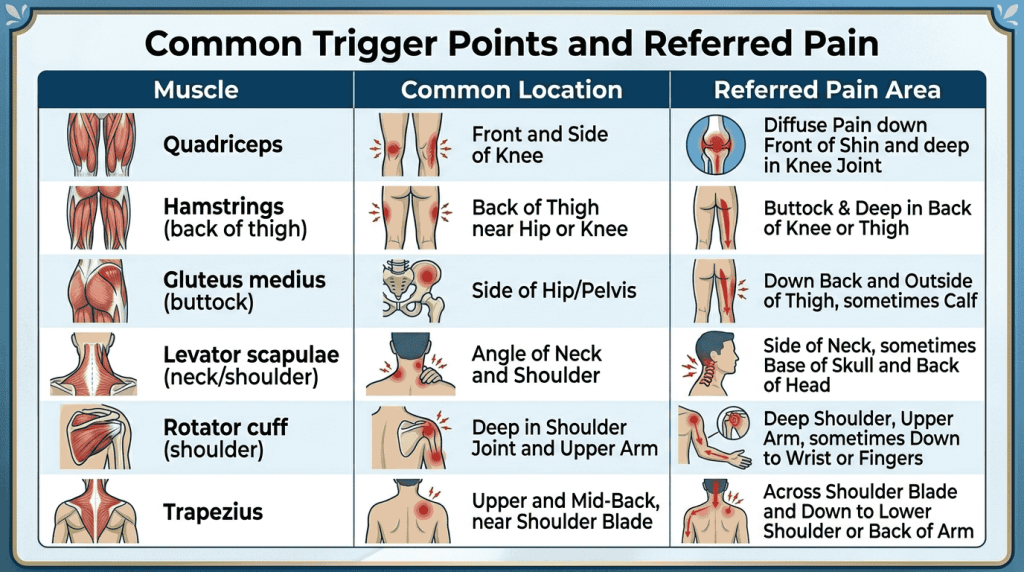
Trigger points are hyperirritable spots located in taut bands of skeletal muscle that produce pain locally and in referred patterns. Pressing on these knots can elicit intense pain and a characteristic local twitch response. Referred pain differentiates trigger points from tender points, which cause pain only at the site of palpation. They may arise after acute trauma or repetitive micro‑trauma, and factors such as poor posture, lack of exercise, or vitamin deficiencies increase the risk of trigger point development.
The relationship between trigger points and joint pain is bidirectional:
A trigger point injection is a minimally invasive procedure in which a small needle is inserted directly into a trigger point to release the muscle spasm. The injectate typically contains:
Trigger point injections target the muscle rather than the joint. In-office treatments involve using a needle to inject lidocaine or another anesthetic into the trigger point to relieve pain. In some practices, fluoroscopy (X‑ray) guidance is used to position the needle precisely; local anesthetic with or without steroid is injected, numbing the trigger point and alleviating pain. The injection may cause a brief cramping or twitch response, but most patients experience immediate muscle relaxation.
Trigger point injections can benefit a wide range of conditions, including:
Trigger points often accompany chronic musculoskeletal disorders and can manifest as tension headaches, temporomandibular joint pain, decreased range of motion in the legs, and low back pain. Identifying and treating these trigger points can help differentiate muscle pain from joint pathology.
During the exam, injections are administered by a qualified practitioner and take about 30 minutes. A small needle is inserted into the trigger point using imaging guidance if necessary, and a local anesthetic (with or without steroid) is injected to numb the trigger point and alleviate pain. Sustained relief is typically achieved with a brief course of treatment, although minor discomfort or a twitch may occur during the injection.
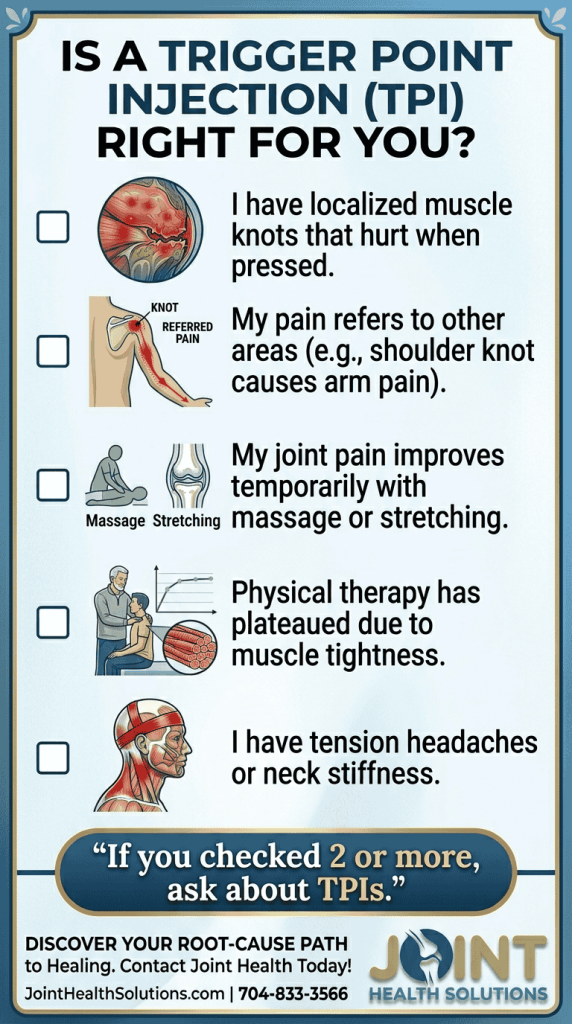
Benefits of trigger point injections include:
Trigger point injections have been demonstrated to inactivate trigger points effectively and can be an adjunctive or primary therapy for musculoskeletal pain. The treatment temporarily relaxes the taut muscle, improves perfusion, and breaks the pain‑tension cycle, leading to improved range of motion and decreased pain. A multimodal approach that includes trigger point injections often yields the best outcomes, and patients can experience significant improvements without relying on pain medications.
Limitations: Trigger point injections treat the muscle component of pain, not the underlying joint pathology. Evidence from clinical trials is limited and suggests a potential placebo effect, so TPIs should be combined with comprehensive care and followed by physical therapy and lifestyle modifications.
Trigger point injections work best as part of a comprehensive plan that may include:
At Joint Health Solutions, we often perform TPIs at the same visit as joint injections – especially for patients with shoulder impingement, knee arthritis, or low back pain – to maximize relief and address multiple pain generators simultaneously.
“Learn more about Trigger Point Injection for Chronic Pain and how it can help relieve muscle knots.”

Most patients feel a brief pinch and a cramping sensation (the twitch response). The discomfort lasts only seconds, and afterward the muscle feels relaxed and soreness is mild.
For acute trigger points, relief can be permanent after one session if the underlying cause is addressed. For chronic myofascial pain, relief may last weeks to months; repeat injections may be needed.
They can eliminate the muscle component of your pain, but if you have underlying arthritis or joint damage, you’ll still need to address that. TPIs are an adjunct, not a standalone cure.
Risks are very low: temporary soreness, bruising or bleeding at the injection site. Rarely, pneumothorax can occur if injecting near the lung, but trained providers take precautions. Severe complications are rare.
It depends. Superficial TPIs may be safe, but we consult your prescribing physician. Never stop blood thinners without approval.
Typically 5–15, depending on the area and your tolerance. We don’t exceed safe doses of anesthetic.
Yes. The local anesthetic wears off within hours and does not impair motor function when used superficially.
Most insurance plans cover TPIs for myofascial pain when medically necessary.
Often both are present. If pressing on a muscle reproduces your pain, trigger points are likely contributing. We can help differentiate during your exam.
Call our office. We’ll evaluate your muscle pain and determine if TPIs are appropriate for you.
Discover the innovative features of our software that streamline your workflow and enhance productivity. With user-friendly interfaces and powerful tools, you can easily manage tasks and collaborate with your team effectively.
Subscribe for wellness tips, treatment updates, and clinic news.
Trusted Expertise
Safe & Effective Care
Built Around You
Local & Accessible
© 2025 Joint Health solutions. All rights reserved.
Discover the innovative features of our software that streamline your workflow and enhance productivity. With user-friendly interfaces and powerful tools, you can easily manage tasks and collaborate with your team effectively.
© 2025 Joint Health solutions. All rights reserved.