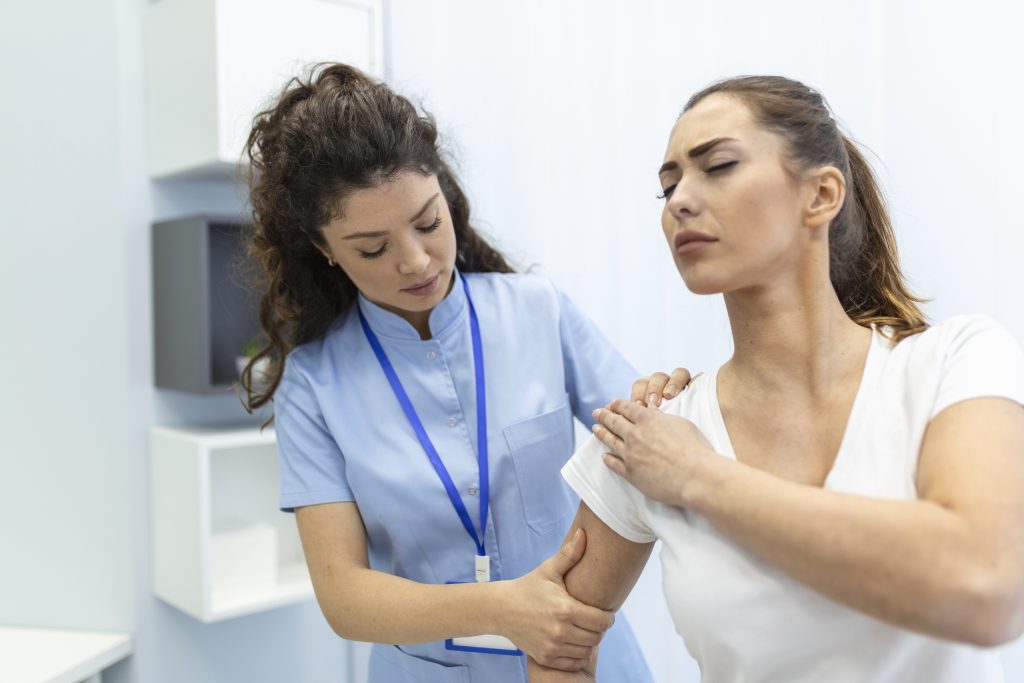
Physical therapy (PT) is one of the most effective, evidence-based treatments for joint pain, osteoarthritis, and musculoskeletal injuries. It focuses on restoring movement, reducing pain, and building strength—without surgery or medication. For many patients, a well-designed physical therapy program can delay or eliminate the need for joint replacement, improve quality of life, and help them return to the activities they love.
At Joint Health Solutions in Charlotte, we view physical therapy as an essential component of comprehensive, non-surgical care. While we offer advanced interventional treatments like PRP therapy, and image-guided injections, we know that lasting results depend on restoring proper movement patterns and building the muscular support around the joint. We work closely with experienced physical therapists to ensure our patients receive personalized, goal-directed rehabilitation.
Medically reviewed by: Dr. Jeffrey Galvin & Ariel Curtis, FNP-C
Physical therapy is a healthcare discipline that uses movement, exercise, manual techniques, and education to improve physical function and reduce pain. Unlike passive treatments such as medication or rest, physical therapy actively engages the patient in their recovery.

How far the joint moves

The capacity of muscles to support the joint
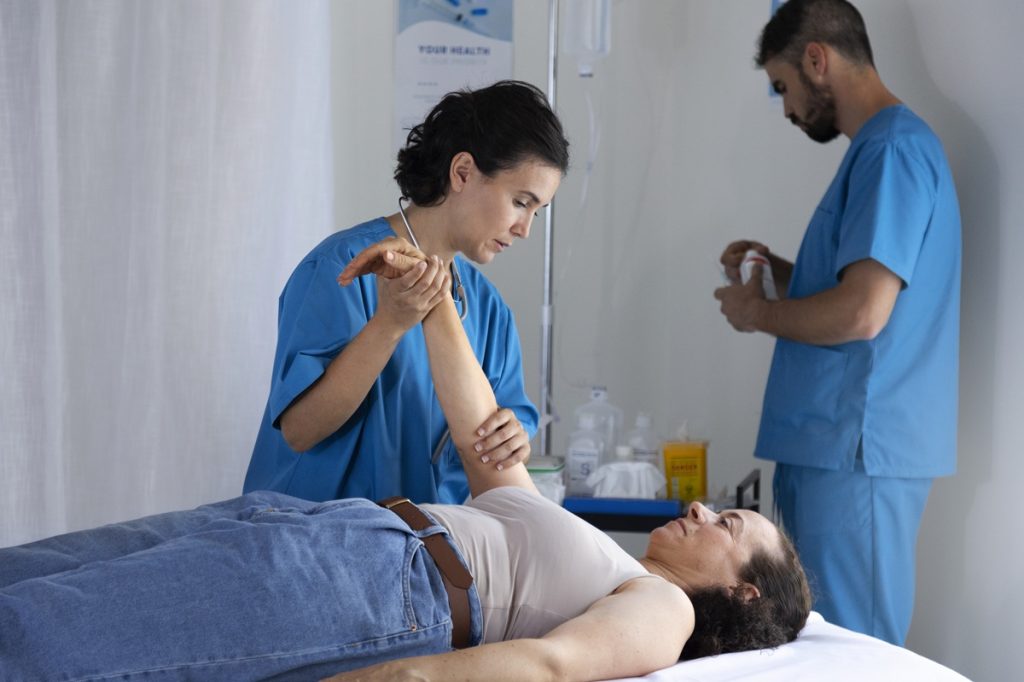
Length of muscles and connective tissues

How you walk, squat, lift, or perform daily tasks

What aggravates or alleviates symptoms
Based on this evaluation, a personalized plan is created. Physical therapy is not a one-size-fits-all prescription; it is tailored to your specific condition, goals, and lifestyle.




| Condition | How PT Helps |
|---|---|
| Knee Osteoarthritis | Strengthens quadriceps; improves gait; reduces load on medial and lateral compartments. |
| Hip Osteoarthritis | Improves hip abductor strength; restores mobility; reduces groin pain. |
| Shoulder Arthritis & Tendinopathy | Restores rotator cuff balance; improves overhead motion; reduces impingement. |
| Low Back Pain & Facet Arthritis | Strengthens core stabilizers; improves posture; reduces segmental stiffness. |
| Cervical Arthritis | Addresses muscle imbalances; improves cervical range of motion. |
| Post-Injury Recovery | After sprains, strains, fractures, or dislocations, PT restores function and prevents recurrence. |
| Pre- & Post-Surgical Rehabilitation | Optimizes outcomes before joint replacement and speeds recovery after surgery. |
| Fibromyalgia & Chronic Pain | Graded exercise and gentle movement reduce central sensitization. |
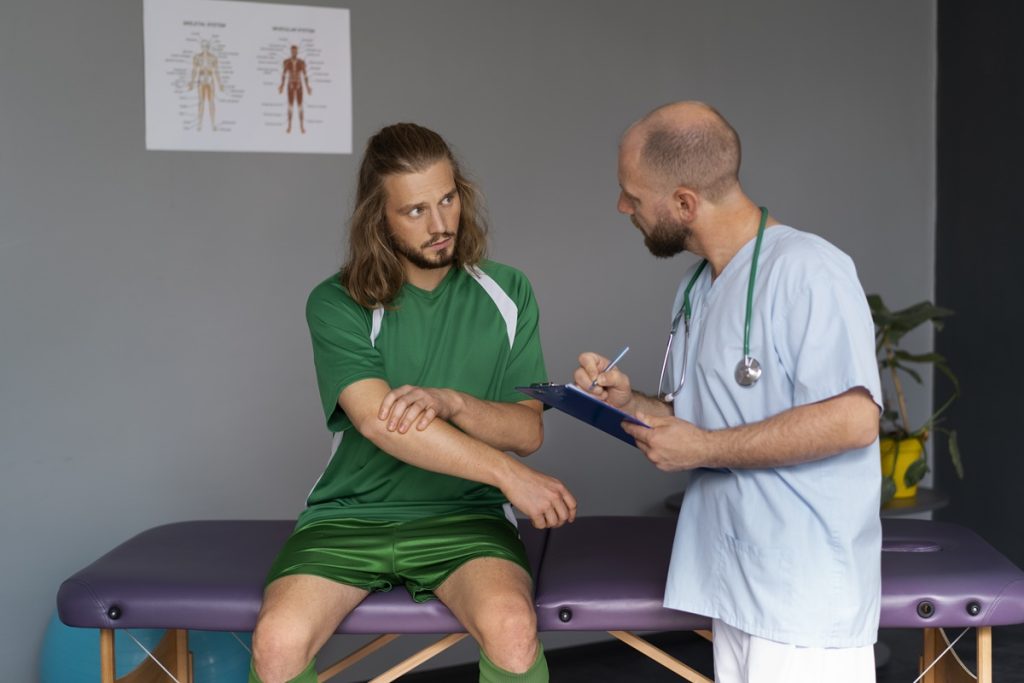
Your journey begins with a thorough evaluation by one of our providers, Dr. Jeffrey Galvin or Ariel Curtis, FNP-C, to diagnose the underlying cause of your pain. We may obtain imaging such as X-rays or ultrasound to understand the condition.
Based on the diagnosis, we prescribe a physical therapy program tailored to your needs. If you work with an external physical therapist, we provide a detailed referral. In some cases, we offer in-house guidance or partner with trusted local PT clinics.
Physical therapy requires active participation. You will be given exercises to perform at home, and you will attend PT sessions to progress your program under the therapist’s guidance. Consistency is key to success.
If you receive injections such as corticosteroids, PRP therapy, physical therapy is timed to maximize benefit. For example, after PRP, we may begin gentle range-of-motion exercises immediately, followed by strengthening once the initial inflammatory phase subsides.
Our goal is to equip you with the tools to manage your condition independently. You will leave with a home exercise program and strategies to protect your joints for years to come.





| Treatment | How It Complements PT |
|---|---|
| Image-Guided Injections (Corticosteroids) | Reduces inflammation to allow pain-free participation in PT. |
| Hyaluronic Acid (Viscosupplementation) | Improves joint lubrication, making movement smoother during PT. |
| PRP (Platelet-Rich Plasma) | Stimulates tissue repair; PT helps remodel tissues into functional strength. |
| IM Toradol | Provides rapid pain relief to enable early mobilization. |
| Anti-Inflammatory IV Therapy | Reduces systemic inflammation, enhancing the body’s response to PT. |
While professional guidance is essential, certain gentle exercises can help maintain joint health. Always consult a provider before starting a new exercise program.
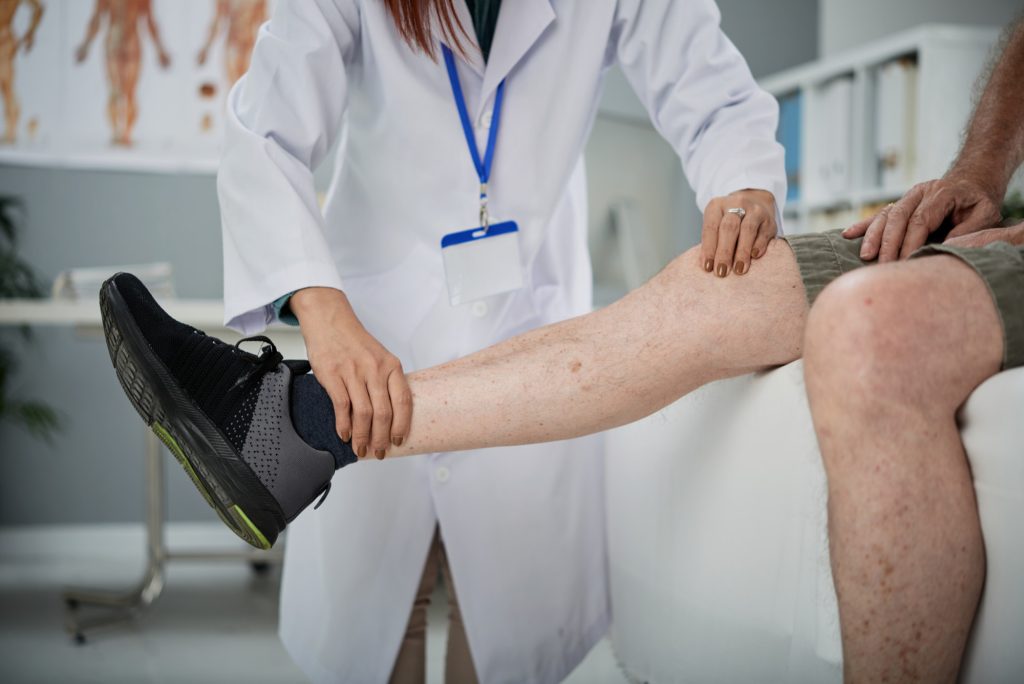



Mild arthritis may improve in 4–6 weeks; chronic conditions may require ongoing maintenance.

Patients who perform home exercises consistently see faster results.
Returning to high-level sports takes longer than achieving pain-free daily activities.
Typical courses range from 4 to 12 weeks of regular sessions, followed by a home-based maintenance program. Some patients benefit from periodic tune-ups to address flare-ups.

We combine physical therapy with advanced interventional and regenerative treatments under one roof.

Accurate diagnosis by Dr. Jeffrey Galvin and Ariel Curtis, FNP-C, ensures your PT program targets the right structures.
Every patient receives a unique prescription based on their specific joint, severity, and goals.

We work closely with trusted physical therapists in Charlotte to ensure seamless communication.
Our goal is to empower you with the tools to manage your joint health for life.
Yes. Physical therapy is one of the most effective non-surgical treatments for osteoarthritis. Strengthening muscles around the joint reduces load on arthritic surfaces, improves stability, and decreases pain. It can delay or even eliminate the need for joint replacement.
In North Carolina, you can see a physical therapist directly (direct access), but many insurance plans require a referral from a physician or specialist. At Joint Health Solutions, we can provide a prescription and work with your physical therapist to ensure coordinated care.
Consistency is more important than intensity. Most home exercise programs are designed to be done daily or every other day. Physical therapy sessions typically occur 1–3 times per week initially, then taper as you progress.
Physical therapy should not cause sharp or worsening pain. You may experience mild soreness after exercise, similar to a good workout, but your therapist will work within a pain-free range. If an exercise causes significant pain, stop and report it.
Many patients notice improvement within 2–4 weeks of consistent physical therapy. Maximum benefits often occur after 6–12 weeks, depending on the severity of the condition and adherence to the program.
Yes. Even with advanced arthritis, physical therapy can help by strengthening the muscles around the joint, improving mechanics, and reducing pain. The focus shifts to avoiding aggravating movements while maintaining as much function as possible.
For many patients, yes. Studies show that physical therapy is as effective as surgery for certain conditions, such as meniscal tears with arthritis, and can significantly delay joint replacement. The key is starting early and being consistent.
Physical therapy focuses on improving movement, strength, and mobility. Occupational therapy focuses on performing daily activities, such as dressing, cooking, and working, and may involve adaptive equipment or techniques. Both can be beneficial for arthritis.
Absolutely. In fact, injections are often used to quiet inflammation so you can engage in physical therapy more comfortably. We carefully time these treatments to maximize synergy.
Wear comfortable, loose-fitting clothing that allows access to the affected joint. For knee or hip issues, shorts are ideal. For shoulder problems, a tank top or loose shirt is helpful. Supportive athletic shoes are recommended.
Ready to take the first step toward pain-free movement? Contact Joint Health Solutions today to schedule an evaluation and receive a personalized physical therapy plan.