The term “bone-on-bone” is one of the most concerning phrases a patient can hear after an X-ray or MRI. It describes the most advanced stage of osteoarthritis, where the protective cartilage that normally cushions the joint has worn away completely, leaving bone surfaces to rub against each other. This condition is often associated with severe pain, chronic inflammation, stiffness, and significant limitations in walking, climbing stairs, or performing everyday activities.
At Joint Health Solutions in Charlotte, we specialize in non-surgical management of advanced osteoarthritis, including bone-on-bone arthritis. While many patients are told that joint replacement is their only option, we offer a range of evidence-based, minimally invasive treatments that can reduce pain, improve function, and in many cases, delay or eliminate the need for surgery. Our approach combines physical therapy, lifestyle modification, image-guided injections, and regenerative medicine to help patients maintain an active, high-quality life.
Medically reviewed by: Dr. Jeffrey Galvin & Ariel Curtis, FNP-C
“Bone-on-bone” is a non-medical term used to describe end-stage osteoarthritis (grade 4 osteoarthritis). In a healthy joint, articular cartilage—a smooth, rubbery tissue—covers the ends of bones, allowing them to glide without friction. In bone-on-bone arthritis, this cartilage is so severely worn that it no longer provides a cushion.

Because bone is richly innervated with pain fibers.
The synovial lining reacts with chronic inflammation.

Range of motion decreases, and joint mechanics are compromised.

Ligaments and muscles weaken due to disuse and abnormal loading.
Despite the advanced nature of bone-on-bone arthritis, many patients can still achieve meaningful relief without surgery. The key is a comprehensive, personalized approach that addresses pain, inflammation, biomechanics, and patient goals.
To understand treatment options, it helps to visualize the changes that occur in end-stage osteoarthritis:
The joint space on X-ray is significantly narrowed or absent.
The bone beneath the cartilage becomes sclerotic (hardened) and may develop cysts.
The body attempts to stabilize the joint by forming extra bone, which can limit motion and cause impingement.
Chronic inflammation leads to swelling, warmth, and the release of enzymes that further degrade joint structures.

Pain causes reduced use, leading to muscle weakness and joint instability.
These changes create a cycle of pain, inactivity, and progressive decline. Interrupting that cycle with targeted non-surgical interventions can restore function and significantly improve quality of life.
The knee is the most common site for end-stage osteoarthritis. Patients often report:
Advanced hip arthritis typically causes:

End-stage glenohumeral (ball-and-socket) arthritis leads to:
While symptoms vary by joint, patients with bone-on-bone arthritis commonly experience:
| Symptom | Description |
|---|---|
| Constant or near-constant pain | Pain may be present even at rest or at night, interfering with sleep. |
| Severe stiffness | Morning stiffness may last more than 30 minutes; the joint may feel “frozen” after inactivity. |
| Swelling and warmth | Chronic synovitis leads to visible swelling and increased warmth around the joint. |
| Crepitus | Loud grinding, crunching, or popping with movement. |
| Loss of motion | Significant reduction in range of motion, often with mechanical block from bone spurs. |
| Instability | The joint may buckle or feel unstable, especially in the knee. |
| Functional limitations | Difficulty with walking, climbing stairs, dressing, lifting, or performing work duties. |
Duration depends on the underlying condition, the severity of inflammation, and whether the injection is part of a comprehensive treatment plan. Some patients achieve lasting relief, while others may need occasional repeat injections.
Diagnosis is typically made through a combination of:
Including prior injuries, symptom progression, and functional limitations.
Assessment of swelling, tenderness, range of motion, crepitus, and stability.

X-rays show loss of joint space, osteophytes, subchondral sclerosis, and cysts. In the knee, a “bone-on-bone” appearance means the joint space is completely absent in one or more compartments. MRI is sometimes used to evaluate soft tissues and confirm the extent of cartilage loss.
At Joint Health Solutions, we also use diagnostic musculoskeletal ultrasound to assess synovitis, effusion, and guide precise injections.
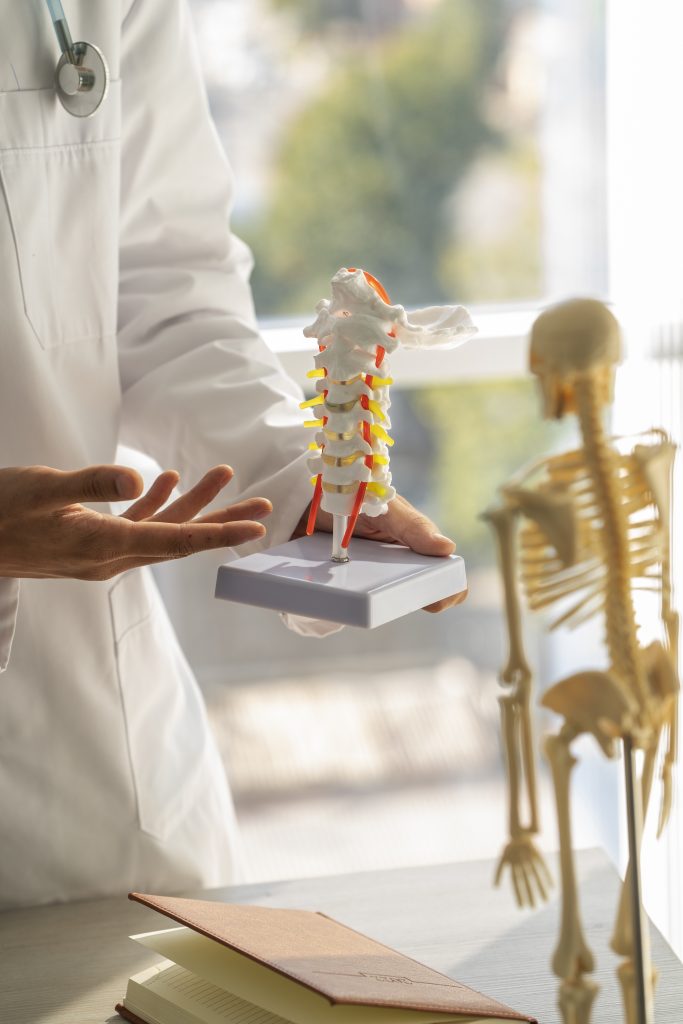
Despite the severity of bone-on-bone arthritis, many patients achieve significant improvement with non-surgical care. Our approach focuses on reducing inflammation, strengthening supporting muscles, optimizing biomechanics, and using advanced injection therapies


For patients with knee or hip arthritis, even a 5-10% reduction in body weight can significantly reduce pain and improve function. Weight loss decreases mechanical load and reduces systemic inflammation.

A targeted physical therapy program focuses on:
Even with bone-on-bone changes, stronger muscles can compensate for joint instability and reduce pain.


Injections are a cornerstone of non-surgical management for advanced arthritis. At Joint Health Solutions, all injections are performed under fluoroscopic or ultrasound guidance to ensure precision, maximize benefit, and minimize risk.
| Injection Type | Mechanism | Best For | Typical Duration |
|---|---|---|---|
| Corticosteroids | Potent anti-inflammatory; reduces synovitis and pain | Acute flare-ups; moderate to severe inflammation | Weeks to months |
| Hyaluronic Acid (Viscosupplementation) | Replaces lubricating joint fluid; provides cushioning | Mild-moderate knee arthritis; some benefit in advanced cases | 6-12 months |
| Platelet-Rich Plasma (PRP) | Concentrated growth factors to modulate inflammation and support tissue health | Advanced arthritis, especially when inflammation is a major component | 6-12+ months |
Note: While no injection can regrow cartilage in a bone-on-bone joint, these therapies can significantly reduce pain, improve function, and delay the need for joint replacement.
Regenerative medicine offers a promising adjunct for patients with advanced osteoarthritis. At Joint Health Solutions, we use:

Derived from the patient’s own blood, PRP contains growth factors and anti-inflammatory cytokines that may help reduce pain and improve joint function even in end-stage arthritis.
These treatments are not guaranteed to reverse bone-on-bone changes, but they can provide meaningful symptom relief and help patients avoid or postpone surgery. Candidacy is determined on a case-by-case basis after thorough evaluation.


Joint replacement (arthroplasty) remains the definitive treatment for end-stage osteoarthritis when conservative options have been exhausted. Surgery is typically considered when:
At Joint Health Solutions, we work with patients to optimize their condition before surgery, and when appropriate, we coordinate with leading orthopedic surgeons in Charlotte to ensure seamless care. Many patients who choose surgery after a period of non-surgical management often experience better postoperative outcomes due to improved muscle strength and pain control.
Non-Surgical Experts
Dr. Jeffrey Galvin and Ariel Curtis, FNP-C, specialize in advanced conservative and interventional treatments for osteoarthritis.
Precision Injections
All procedures are performed with fluoroscopic or ultrasound guidance for accuracy, safety, and optimal results.
Comprehensive Approach
We combine physical therapy, lifestyle modification, injection therapies, and regenerative medicine to address the full spectrum of the disease.
Personalized Care
Your treatment plan is customized based on your specific joint, severity, goals, and lifestyle.
Local Convenience
Serving Charlotte and surrounding areas including Huntersville, Concord, Matthews, and Cornelius.
Yes. Many patients with bone-on-bone arthritis achieve significant pain relief and functional improvement with non-surgical treatments such as physical therapy, bracing, image-guided injections (cortisone, hyaluronic acid, PRP), and regenerative medicine. While surgery remains an option for those who do not respond, a well-structured conservative approach can often delay or eliminate the need for joint replacement.
PRP (platelet-rich plasma) has been shown to reduce pain and improve function in patients with moderate to severe osteoarthritis, including some with bone-on-bone changes. PRP works by delivering concentrated growth factors that reduce inflammation and may support the health of remaining joint tissues. While it does not regrow cartilage, it can provide meaningful relief and improve quality of life.
The number of injections depends on the treatment type and your response. Corticosteroid injections may be repeated every 3-4 months as needed. Hyaluronic acid is typically a series of 1-3 injections. PRP often involves 1-3 treatments spaced several weeks apart. Your provider will develop a plan based on your specific condition.
Absolutely. Physical therapy is essential for managing bone-on-bone arthritis. Strengthening the muscles around the joint helps stabilize it, reducing the load on the arthritic surfaces. Improved flexibility and movement patterns can decrease pain and improve function, even in advanced stages.
Many patients delay joint replacement for years with a combination of lifestyle modifications, physical therapy, and periodic injections. Some patients avoid surgery altogether. The duration depends on the severity of symptoms, the joint involved, and how well you respond to treatment.
Yes. Weight loss is one of the most effective interventions for knee and hip arthritis. Every pound of body weight lost reduces the load on the knee by approximately 4 pounds during walking. A 10% reduction in body weight can significantly decrease pain and improve function.
Walking is generally beneficial if it does not cause a significant increase in pain. It maintains joint mobility, strengthens muscles, and supports cardiovascular health. If walking is painful, consider shorter distances, flat surfaces, supportive footwear, or using a cane. Alternative low-impact activities like cycling or swimming may be recommended.
Most patients with bone-on-bone arthritis are candidates for non-surgical treatment unless they have a surgical emergency (such as a fracture) or a condition that makes conservative care unsafe. A comprehensive evaluation-including history, physical exam, and imaging-will determine which treatments are appropriate for you.
Success depends on the definition. Many patients achieve meaningful pain reduction, improved function, and satisfaction that allows them to postpone or avoid surgery. Success is highest when patients actively participate in their treatment plan, including physical therapy, weight management, and following activity recommendations.
If you’ve been told you have bone-on-bone arthritis and want to explore non-surgical treatment options in Charlotte, schedule an evaluation today.
Request an appointment online: Schedule Now