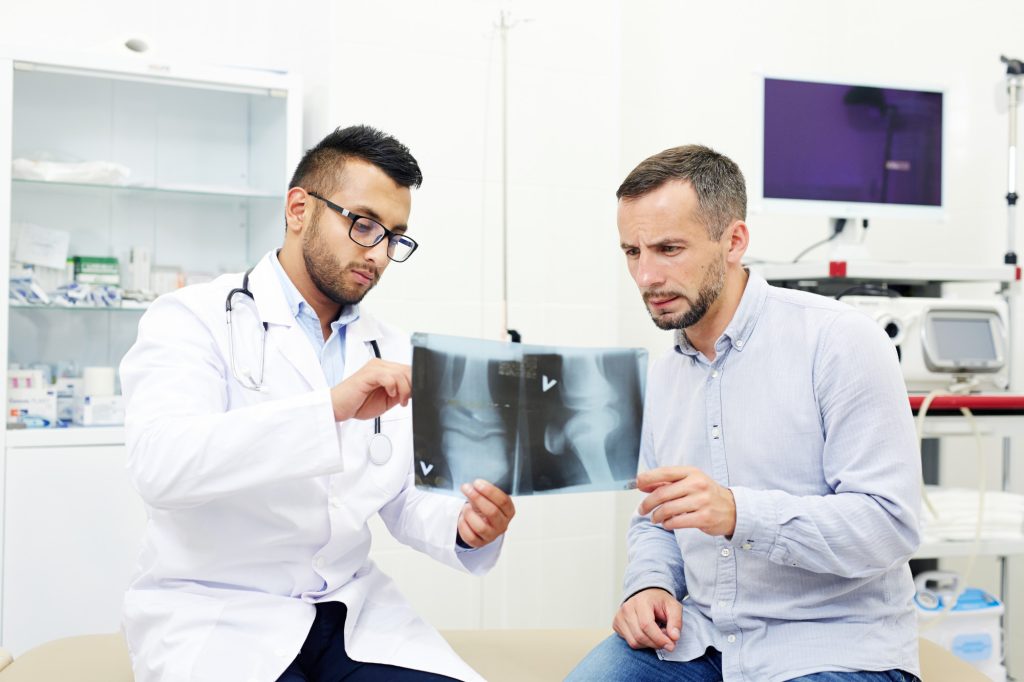
Degenerative joint disease (DJD), commonly known as osteoarthritis, is the most common form of arthritis and a leading cause of chronic pain and disability. It occurs when the protective cartilage that cushions the ends of bones gradually wears away, leading to pain, stiffness, swelling, and reduced mobility.
At Joint Health Solutions in Charlotte, we specialize in non-surgical management of degenerative joint disease. Our approach focuses on relieving pain, improving joint function, and helping patients stay active without relying on surgery or long-term medication. Whether your symptoms affect the knees, hips, shoulders, or spine, we develop a personalized treatment plan using evidence-based therapies, including physical therapy, image-guided injections, and regenerative medicine when appropriate.
Medically reviewed by: Dr. Jeffrey Galvin & Ariel Curtis, FNP-C
Degenerative joint disease (DJD), also called osteoarthritis or wear-and-tear arthritis, is a progressive condition that affects the synovial joints. It involves the breakdown of articular cartilage, changes in the subchondral bone, formation of bone spurs (osteophytes), and inflammation of the joint lining (synovium).
Unlike systemic inflammatory arthritis (such as rheumatoid arthritis), DJD is localized to the affected joints and is driven by mechanical stress, aging, and cumulative micro-injury. While DJD is often associated with aging, it can also develop after joint trauma, in people with obesity, or in those with genetic predispositions.

In a healthy joint, smooth cartilage covers the bone ends, allowing friction-free movement. Synovial fluid lubricates the joint and nourishes the cartilage.
With degenerative joint disease:
These changes result in progressive pain, stiffness, and functional decline.
DJD can affect any synovial joint, but certain areas are most commonly impacted.
The knee is one of the most frequently affected joints due to its weight-bearing role. Symptoms include pain with walking, climbing stairs, stiffness after sitting, swelling, and occasional buckling.

Hip DJD often causes deep groin pain, outer hip discomfort, and difficulty with activities like putting on shoes or rising from a seated position. Stiffness and a limp may develop over time.

Shoulder arthritis leads to pain with overhead motion, reaching, and lifting. Patients may notice crepitus (grinding), reduced range of motion, and difficulty sleeping on the affected side.
Degenerative changes in the spine affect the facet joints and intervertebral discs. This can cause localized neck or back pain, stiffness, and sometimes radiating pain if nerve roots are involved.

DJD in the hands often involves the base of the thumb, the distal finger joints (Heberden’s nodes), and the middle finger joints (Bouchard’s nodes). Grip strength and fine motor tasks become challenging.
Symptoms vary depending on the joint and severity but commonly include:
Pain – Typically worsens with activity and improves with rest; in advanced stages, pain may be constant or nocturnal.
Stiffness – Morning stiffness lasting less than 30 minutes; stiffness after inactivity (gelling phenomenon).
Swelling – Intermittent or persistent joint effusion.
Crepitus – Grinding, cracking, or popping sensation with movement.
Reduced range of motion – Difficulty performing daily activities.
Instability – The joint may feel weak or give way, especially in the knee.
Functional limitations – Difficulty walking, climbing stairs, lifting, or reaching.
| Risk Factor | Explanation |
|---|---|
| Age | Prevalence increases significantly after age 50. |
| Obesity | Excess weight increases mechanical load and promotes systemic inflammation. |
| Previous joint injury | Fractures, ligament tears, meniscal injuries, or dislocations predispose to post-traumatic DJD. |
| Repetitive stress | Occupations or sports with repetitive joint loading accelerate cartilage wear. |
| Genetics | Family history of DJD or congenital joint abnormalities (e.g., hip dysplasia). |
| Muscle weakness | Weak supporting muscles fail to stabilize the joint, increasing stress on cartilage. |
| Joint malalignment | Bowlegs, knock-knees, or scoliosis create uneven load distribution. |