You’ve probably noticed that your joint pain flares up during stressful times – a big work deadline, family conflict, or financial worries. This isn’t just in your head. There’s a powerful biological connection between stress and joint pain.
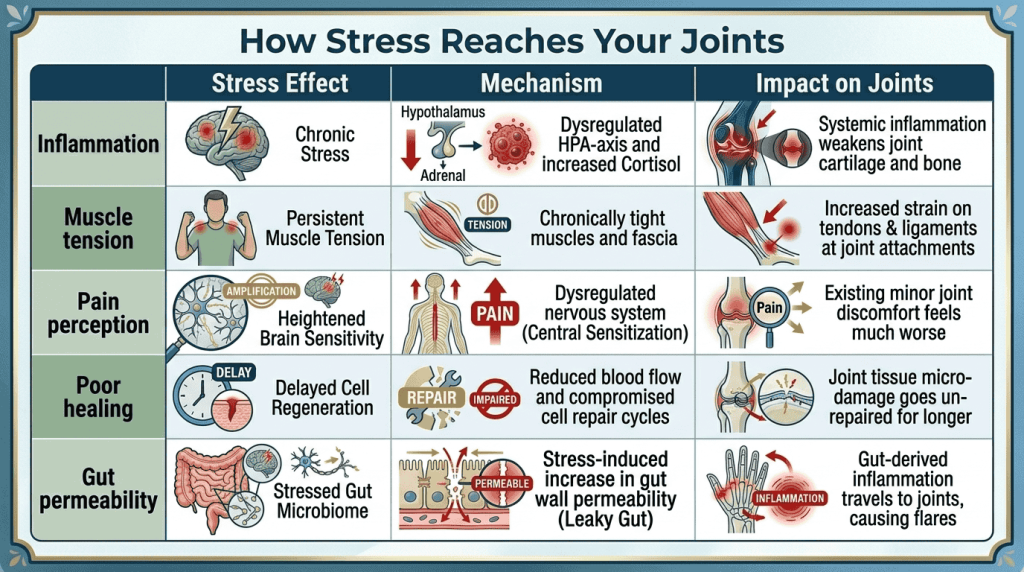
Chronic stress keeps your body in a constant state of “fight or flight,” flooding it with stress hormones like cortisol and adrenaline. Over time, this leads to systemic inflammation, muscle tension, altered pain perception and impaired healing – all of which worsen arthritis and other joint conditions.
At Joint Health Solutions, we address stress as a critical component of our root‑cause approach. In this article, we’ll explain how stress affects your joints and share practical, evidence‑based strategies to break the stress‑pain cycle.
When you perceive a threat, your body activates the sympathetic nervous system and releases cortisol and adrenaline. This response is designed to be short‑lived, preparing you to run or fight. However, chronic stress – whether from work, relationships, financial strain, or illness – keeps this system activated. Persistent high cortisol leads to several problems that directly impact joint health, including immune dysregulation, chronic muscle tension, disrupted sleep, hormonal imbalances and increased gut permeability.
Chronic stress increases the production of pro‑inflammatory cytokines (such as IL‑6 and TNF‑alpha) and elevates CRP levels. Elevated cortisol also reduces the body’s ability to regulate inflammation, creating a vicious cycle where stress begets inflammation and inflammation worsens joint pain.
Under stress, muscles contract and remain tight. Over time, this leads to trigger points, muscle fatigue and altered joint mechanics. Chronic tension in the shoulders, back or legs can exacerbate impingement, patellar tracking problems and other joint conditions.
Stress lowers your pain threshold and amplifies pain signals in the central nervous system (central sensitization). This means you may feel arthritis pain more intensely than the actual joint damage would suggest.
Cortisol impairs tissue repair by reducing collagen synthesis and slowing cell turnover. Chronic stress disrupts cytokine signalling and fibroblast function; studies show glucocorticoids can reduce type I and III collagen mRNA by 70% and collagen production by 80%, which delays healing of meniscal tears, cartilage defects and tendon injuries.
The gut‑brain axis plays a critical role in joint health. Chronic stress increases intestinal permeability (“leaky gut”) and alters the gut microbiome, allowing bacterial toxins like lipopolysaccharide (LPS) to enter the bloodstream. These toxins trigger systemic inflammation that often lands in joints, even in people without pre‑existing arthritis.
Stress also reduces vagal tone – the ability of the vagus nerve to dampen inflammation – further exacerbating joint pain. Because gut and joint health are tightly linked, our functional medicine evaluations include assessments of gut permeability and microbiome balance.
Learn more about how gut health influences joint pain in our article on gut health and joint pain.
You can’t eliminate all stress from your life, but you can change how you respond to it. Evidence‑based techniques reduce cortisol, lower inflammation and improve joint pain.
Mindfulness meditation – 10–20 minutes daily reduces CRP and pain catastrophizing.
Deep breathing (diaphragmatic breathing) – Activates the vagus nerve, lowering inflammation.
Progressive muscle relaxation – Reduces muscle tension and improves sleep.
Yoga or Tai Chi – Combines gentle movement, breathing and meditation; shown to reduce arthritis pain.
Poor sleep elevates cortisol and inflammatory markers. Aim for 7–9 hours of quality sleep:
• Maintain a consistent sleep schedule (even on weekends).
• Avoid screens 1 hour before bed.
• Keep your bedroom cool, dark and quiet.
• Avoid caffeine after 2 PM and alcohol before bed.
• Consider magnesium glycinate or melatonin (consult your provider).
Regular low‑impact exercise reduces stress hormones and releases endorphins. Aim for:
• 150 minutes per week of moderate activity (walking, swimming, cycling).
• Gentle stretching daily.
• Avoid overtraining – excessive exercise can raise cortisol.
Isolation worsens pain and stress. Stay connected:
• Schedule regular calls or visits with friends or family.
• Join a support group (in‑person or online) for arthritis or chronic pain.
• Consider therapy or counseling if you’re feeling overwhelmed.

Stress management isn’t a replacement for medical treatments – it’s a force multiplier that makes everything else work better.
• Before joint injections (PRP, cortisone, HA): Lower stress improves healing outcomes.
• During physical therapy: Relaxed muscles respond better to stretching and strengthening.
• After surgery: Stress reduction speeds recovery and reduces complication risk.
• We can help you integrate stress management into your personalized plan. This may include referrals to mindfulness‑based stress reduction (MBSR) programs, biofeedback or heart rate variability training, supplements that support stress resilience (ashwagandha, L‑theanine, magnesium) and addressing underlying sleep disorders (sleep apnea, insomnia).
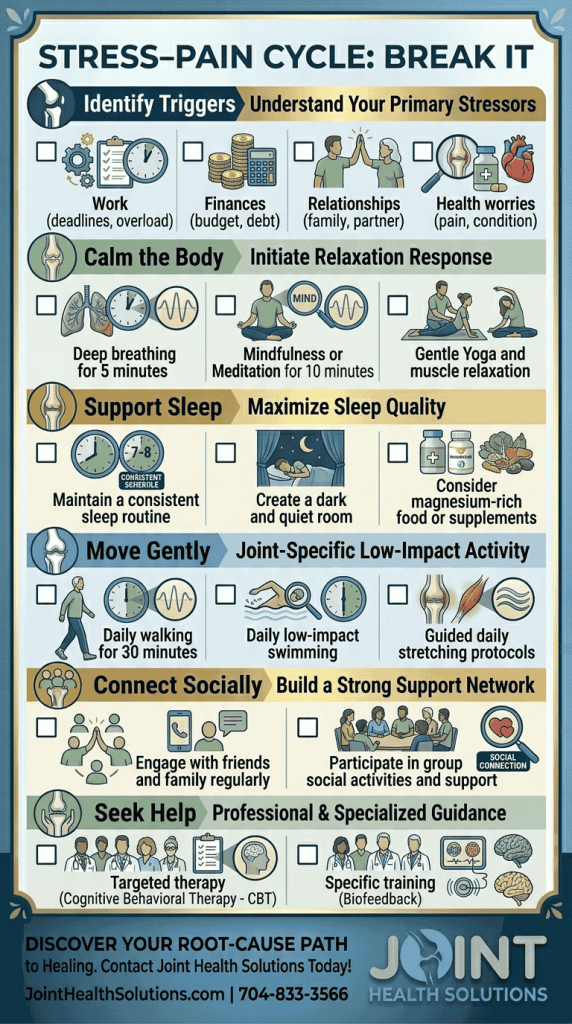
If stress is overwhelming and self‑help strategies aren’t enough, professional support can make a difference. Consider therapy (cognitive behavioural therapy or acceptance and commitment therapy), biofeedback, short‑term use of anxiolytics or antidepressants under supervision, and structured stress management programs. Addressing stress is not a sign of weakness – it’s a critical part of treating your joint pain.
Yes. Stress‑induced inflammation and muscle tension can cause joint pain in people with no underlying joint disease. However, if pain persists, you should be evaluated for arthritis.
Some patients notice improvement within 1–2 weeks of consistent practice (e.g., daily meditation, better sleep). Full benefits may take 4–8 weeks.
Mindfulness meditation has the strongest evidence for reducing pain and inflammation. However, the best technique is the one you’ll actually do daily.
Yes. Chronic stress accelerates cartilage loss and may increase the risk of developing autoimmune arthritis.
Absolutely. Stress increases leaky gut, which allows inflammatory toxins to reach your joints. Healing the gut is part of breaking the cycle.
Ashwagandha, L‑theanine, magnesium glycinate and omega‑3s have evidence for reducing stress and inflammation. Always consult your provider before starting supplements.
Poor sleep elevates cortisol and inflammatory markers, lowers pain threshold and impairs tissue repair. Improving sleep is one of the most effective ways to reduce joint pain.
Overtraining or high‑intensity exercise can raise cortisol. Stick to low‑to‑moderate intensity (you should be able to talk while exercising) and listen to your body.
Not usually, but it can reduce the frequency and intensity of flares and may improve the durability of injection results.
Call our office. We can assess your stress levels, recommend techniques and refer you to appropriate resources.
Arthritis Foundation – Stress and Arthritis – https://www.arthritis.org/health-wellness/healthy-living/emotional-well-being/stress-management/stress-and-arthritis
Harvard Health Publishing – The gut‑brain connection – https://www.health.harvard.edu/diseases-and-conditions/the-gut-brain-connection
Cleveland Clinic – Stress and Inflammation – https://my.clevelandclinic.org/health/articles/11874-stress-and-inflammation
Cleveland Clinic – How stress affects your body – https://my.clevelandclinic.org/health/articles/13798-stress-and-your-body
Arthritis Australia – Stress and Arthritis – https://www.arthritis.org.au/your-health/living-with-arthritis/managing-your-arthritis/stress-and-arthritis
Dermatology Times – Stress and wound healing – https://www.dermatologytimes.com/view/impact-stress-cutaneous-wound-healing
OMED Health – Stress and gut health – https://omedhealth.com/blog/stress-and-gut-health
Discover the innovative features of our software that streamline your workflow and enhance productivity. With user-friendly interfaces and powerful tools, you can easily manage tasks and collaborate with your team effectively.
Subscribe for wellness tips, treatment updates, and clinic news.
Trusted Expertise
Safe & Effective Care
Built Around You
Local & Accessible
© 2025 Joint Health solutions. All rights reserved.
Discover the innovative features of our software that streamline your workflow and enhance productivity. With user-friendly interfaces and powerful tools, you can easily manage tasks and collaborate with your team effectively.
© 2025 Joint Health solutions. All rights reserved.