Joint injections are one of the most effective non-surgical tools for managing pain, reducing inflammation, and improving joint function. Whether you suffer from osteoarthritis, tendonitis, bursitis, or persistent joint pain, a precisely placed injection can provide relief and help you avoid or delay surgery.
At Joint Health Solutions in Charlotte, we specialize in advanced, image-guided joint injections. Our team—led by Dr. Jeffrey Galvin and Ariel Curtis, FNP-C—uses state-of-the-art ultrasound and fluoroscopy to ensure every injection is delivered with pinpoint accuracy, maximizing benefit and minimizing risk. We offer a full range of injection therapies, from traditional corticosteroids to cutting-edge regenerative medicine such as PRP.
Medically reviewed by: Dr. Jeffrey Galvin & Ariel Curtis, FNP-C
Joint injections are minimally invasive procedures in which medication is delivered directly into a joint, bursa, or tendon sheath to treat pain and inflammation. By targeting the source of discomfort, injections often provide faster and more effective relief than oral medications.
Joint injections can serve multiple purposes:

Reduce inflammation, relieve pain, and improve function.
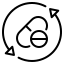
Help confirm the source of pain when imaging and physical exam are inconclusive.

Stimulate the body’s own healing processes to repair damaged tissues.
Arthritis can affect one, two, or all three compartments. Understanding which compartments are involved helps guide treatment.
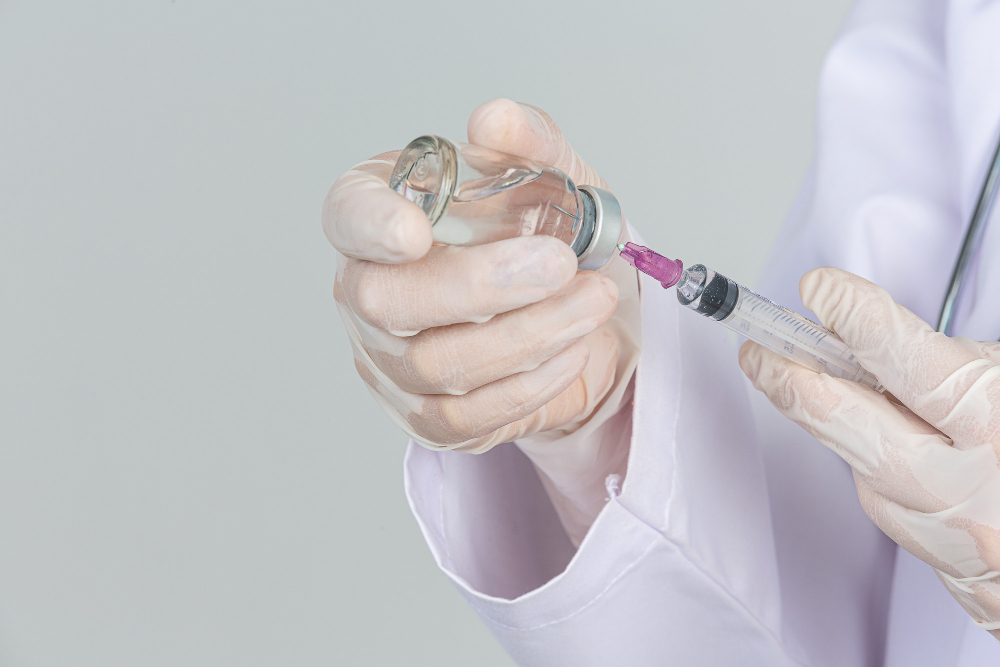
Corticosteroids, commonly called steroid shots, are powerful anti-inflammatory medications that rapidly reduce swelling, redness, and pain. They are typically used for acute flare-ups of arthritis, bursitis, tendonitis, and other inflammatory conditions.

Hyaluronic acid is a naturally occurring substance in joint fluid that provides lubrication and shock absorption. In osteoarthritis, the natural hyaluronic acid becomes diluted and less effective. Injecting a gel-like supplement can improve joint lubrication, reduce pain, and improve mobility.
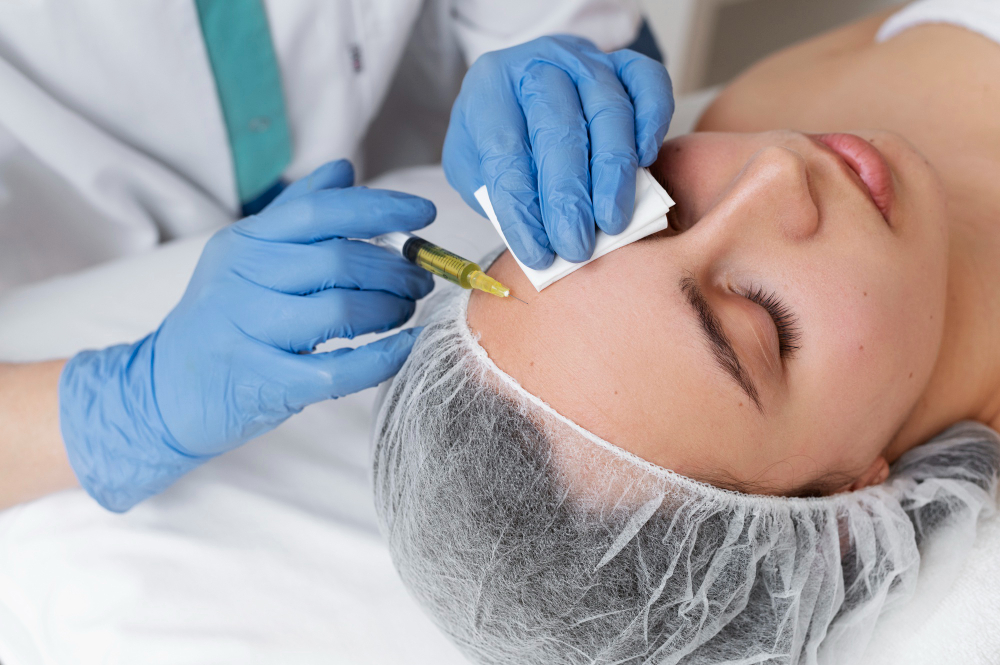
PRP is a regenerative therapy made from a small sample of your own blood. The blood is processed to concentrate platelets, which contain growth factors that reduce inflammation and stimulate tissue repair. PRP is used for osteoarthritis, tendonitis, and ligament injuries.
| Injection Type | Mechanism of Action | Best For | Typical Duration |
|---|---|---|---|
| Corticosteroids | Suppress inflammation by inhibiting inflammatory cytokines and immune cells. | Osteoarthritis flare-ups, bursitis, and tendonitis. | Weeks to months |
| Hyaluronic Acid | Restores joint fluid viscosity, improves lubrication, and may reduce inflammation. | Mild to moderate knee osteoarthritis. | 6–12 months |
| PRP | Delivers concentrated growth factors that modulate inflammation and promote tissue repair. | Mild to moderate arthritis and ligament injuries. | 6–12+ months |
All injections are performed under image guidance—ultrasound or fluoroscopy—to ensure the medication is delivered exactly where it is needed into the joint space, bursa, or tendon sheath.
Knee, hip, shoulder and spine facet joints
Adjunctive therapy for inflamed joints
Subacromial, trochanteric, olecranon, and prepatellar bursitis
Rotator cuff, patellar, Achilles, and tennis elbow conditions
Corticosteroid injections for symptom relief
Aspiration and injection
Corticosteroid or PRP injections
Spine injections for neck or back pain
Corticosteroid or PRP injections
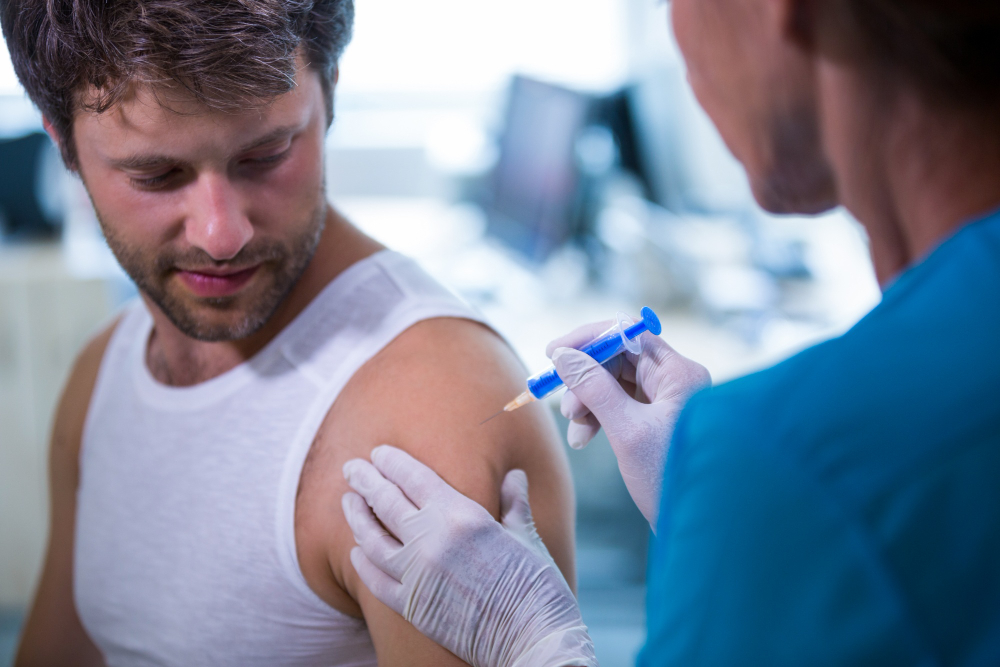

Ensures medication reaches the exact target, improving effectiveness.
Avoids accidental injection into blood vessels, nerves, or surrounding tissues.
Real-time imaging allows us to see inflammation, fluid, or structural abnormalities.
Ultrasound is especially useful for soft-tissue structures such as tendons and bursae, while fluoroscopy is preferred for deeper joints like the hip or spine.
Your care begins with a comprehensive evaluation by one of our providers. We review your medical history, perform a focused physical exam, and review any available imaging. We determine whether an injection is appropriate and which type best suits your condition.
On the day of the injection, you will be positioned comfortably. The skin over the injection site is cleansed with an antiseptic. For some procedures, a local anesthetic is used to numb the area.
Using ultrasound or fluoroscopy, we identify the target joint, bursa, or tendon. A small needle is guided precisely to the target, and the medication is injected. The process typically takes 5–15 minutes.
You will be observed briefly and then discharged with specific instructions. For corticosteroid injections, you may be advised to rest the joint for 24–48 hours. For PRP therapy, you may need to avoid anti-inflammatory medications and limit activity for a short period.
We discuss all risks with you before the procedure and take every precaution to ensure safety.
| Injection Type | Typical Duration of Relief |
|---|---|
| Corticosteroids | Weeks to months |
| Hyaluronic Acid | 6–12 months |
| PRP (Platelet-Rich Plasma) | 6–12+ months |
Duration depends on the severity of the underlying condition, the joint involved, and individual patient factors. Some patients achieve lasting relief, while others may benefit from periodic maintenance injections.
Dr. Jeffrey Galvin and Ariel Curtis, FNP-C, have extensive training in interventional pain management and regenerative medicine.
All injections are performed under ultrasound or fluoroscopy for accuracy and safety.
We offer a full spectrum of injection therapies, from traditional to regenerative.
Your treatment plan is tailored to your specific condition, goals, and lifestyle.
Your treatment plan is tailored to your specific condition, goals, and lifestyle.
Serving patients from Charlotte, Huntersville, Concord, Matthews, and surrounding areas.
Most patients feel a brief pinch or pressure during the injection. The procedure is typically well tolerated. If needed, we can use local anesthetic to numb the area. After the injection, some patients experience mild soreness for a day or two.
Corticosteroids often begin working within 24–72 hours, though full effect may take up to a week. Hyaluronic acid may take 2–4 weeks. PRP often causes initial soreness followed by gradual improvement over several weeks to months.
It depends on the type of injection and your condition. Corticosteroids are often used as needed for flare-ups. Hyaluronic acid is usually a series of 1–3 injections. PRP therapy typically involve 1–3 treatments, often spaced several weeks apart.
Corticosteroid and hyaluronic acid injections are often covered by insurance. PRP therapy are typically considered elective and are not covered. We provide transparent pricing and can discuss financing options.
For corticosteroid injections, we usually recommend resting the joint for 24–48 hours. For PRP therapy, we may advise avoiding anti-inflammatory medications and limiting strenuous activity for a short period. You will receive specific post-injection instructions.
To minimize the risk of cartilage damage, we typically limit corticosteroid injections to 3–4 times per year in the same joint. The goal is to use them strategically for flare-ups while building a long-term plan with physical therapy and other modalities.
It depends on the situation. Cortisone provides rapid relief of acute inflammation and is excellent for flare-ups. PRP works more slowly but may offer longer-lasting improvement by addressing the underlying inflammatory process and promoting tissue repair. Sometimes we use both strategically at different times.
It depends on the type of blood thinner and the risk of bleeding. Some patients may need to temporarily hold their medication with approval from their prescribing physician, while others may be candidates for injection with special precautions. We review each case individually.
Ultrasound uses sound waves to visualize soft tissues such as tendons, bursae, and fluid, and is ideal for most shoulder, knee, and soft-tissue injections. Fluoroscopy uses real-time X-ray to visualize bone and joint spaces, making it ideal for deep joints like the hip or spine.
You may be a candidate for a joint injection if you have persistent joint pain that limits daily activities, oral medications provide inadequate relief or cause side effects, you are experiencing an acute flare-up of arthritis or bursitis, you want to avoid or delay joint replacement surgery, or you need pain relief to participate more effectively in physical therapy.
If you are considering a joint injection for arthritis, tendonitis, or chronic joint pain, schedule a consultation at Joint Health Solutions in Charlotte. We will help you determine the best approach for your needs.