This article is for educational purposes only. It is not medical advice, and it does not imply that Joint Health Solutions offers food sensitivity testing, elimination diets, or nutritional counseling. We do not perform any type of food allergy or sensitivity testing. We do not provide gluten sensitivity testing, celiac disease testing, or dietary management. If you suspect a food triggers your joint pain, please consult your primary care provider or a registered dietitian. Do not start an elimination diet before being properly evaluated for conditions like celiac disease.
Many people living with chronic joint pain – whether from osteoarthritis, rheumatoid arthritis, or other conditions – wonder whether something they eat could be making their symptoms worse. The short answer is: possibly, but it depends on the individual. There is no single “arthritis diet” that works for everyone.
However, research over the past two decades has identified certain foods and dietary patterns that may promote systemic inflammation, which could worsen pain in susceptible individuals. This guide summarizes what scientific studies have found about the connection between diet and joint pain, focusing on common triggers like gluten, dairy, and sugar.
Inflammation is a normal immune response, but chronic, low-grade systemic inflammation is a known driver of pain in many forms of arthritis. In osteoarthritis, inflammatory cytokines contribute to cartilage breakdown , while in rheumatoid arthritis, the immune system directly attacks joint tissues.
Certain dietary components can influence these inflammatory markers. For example, high sugar intake is associated with higher C-reactive protein (CRP) levels , while omega-3 fatty acids found in fish can reduce inflammatory cytokines. While diet is not a cure and cannot reverse structural damage, identifying triggers may improve quality of life.
The following table summarizes foods that have been studied for their potential role in joint pain. Evidence varies; individual responses differ.
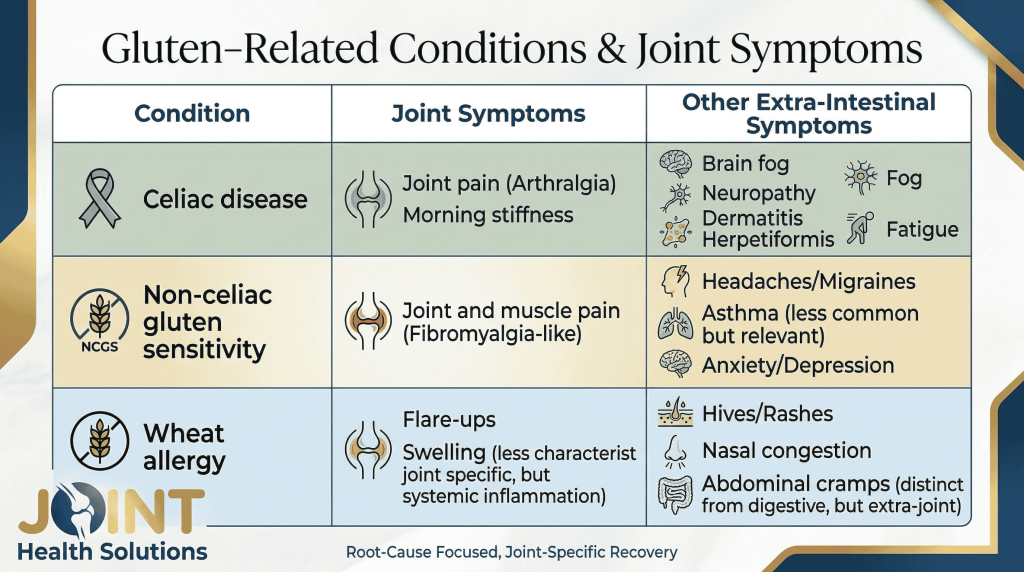
Gluten is a protein that triggers an autoimmune response in people with celiac disease (about 1% of the population). However, a larger group – estimated at 6‑10% of the population – may have non‑celiac gluten sensitivity (NCGS) . People with NCGS do not have intestinal damage, but they can experience extra‑intestinal symptoms including joint pain, brain fog, fatigue, and headaches – sometimes without any digestive issues.
A 2022 review in the journal Nutrients concluded that NCGS is a real clinical entity, and joint pain is one of the most commonly reported extra‑intestinal symptoms. However, there is no single blood test for NCGS. Diagnosis is made by ruling out celiac disease and wheat allergy, followed by a gluten elimination and challenge under medical supervision.
What you should know: If you suspect gluten is affecting your joints, do not start a gluten‑free diet before being tested for celiac disease. Celiac blood tests require you to be eating gluten for 2‑6 weeks. Going gluten‑free first can cause false negatives. Discuss this with your primary care provider or a gastroenterologist.
Some individuals report increased joint pain after consuming milk, cheese, or yogurt. This may be due to casein (a milk protein) or lactose intolerance. However, research evidence is mixed. A few small studies have suggested that a subgroup of people with rheumatoid arthritis may benefit from a dairy‑free diet, but most people with osteoarthritis see no difference. A 2019 systematic review found no consistent evidence linking dairy consumption to increased inflammation in healthy adults.
What you should know: If you suspect dairy is a trigger, you can try a short elimination trial (under a doctor’s guidance) – typically 2‑4 weeks without dairy, followed by reintroduction while tracking symptoms. Keep a symptom diary.
High intake of added sugar (soda, candy, pastries) and refined carbohydrates (white bread, white rice, pasta made from white flour) can spike blood sugar and increase the production of inflammatory cytokines. Several observational studies have found that higher sugar consumption is associated with higher levels of C‑reactive protein (CRP) , a marker of systemic inflammation. A 2018 study in the American Journal of Clinical Nutrition reported that reducing sugary beverages significantly lowered inflammatory markers in overweight adults.
What you should know: Reducing added sugar is a reasonable general health goal for anyone with chronic pain. The Dietary Guidelines for Americans recommend limiting added sugar to less than 10% of daily calories. However, sugar reduction is not a cure for arthritis.
Nightshades contain a compound called solanine, which has been anecdotally reported to worsen arthritis symptoms. Some online sources strongly warn against nightshades. However, scientific evidence is lacking. A 2018 review in Current Rheumatology Reports found no consistent association between nightshade consumption and increased joint pain. In fact, tomatoes are rich in lycopene, an antioxidant that may reduce inflammation.
What you should know: Some individuals may be sensitive to nightshades, but for most people, they are safe and nutritious. If you suspect nightshades are a problem, you can try eliminating them for 4 weeks and then reintroducing them – but keep a symptom diary. Do not eliminate entire food groups without medical reason.
Highly processed foods (fast food, frozen meals, packaged snacks, vegetable oils like corn and soybean oil) are often high in omega‑6 fatty acids and low in omega‑3s. An imbalance between omega‑6 and omega‑3 can promote inflammation. The typical Western diet has an omega‑6 to omega‑3 ratio of 15:1 or higher, whereas a ratio of 4:1 or lower is considered more anti‑inflammatory.
What you should know: Reducing processed foods and increasing omega‑3 rich foods (fatty fish: salmon, sardines, mackerel; walnuts; flaxseeds) is generally recommended for overall health. However, this does not replace medical treatment for arthritis.
The Mediterranean diet is widely recommended, characterized by high consumption of fruits, vegetables, whole grains, and extra virgin olive oil. If you are looking for additional ways to manage discomfort, you can explore IV therapy for inflammation.
No. Diet is not a cure for arthritis and it cannot reverse structural damage like cartilage loss. However, it can help manage systemic inflammation. To address structural issues, you may want to learn about PRP therapy.
Not necessarily. Scientific reviews find no consistent association between nightshades and increased joint pain. Unless you personally notice a flare-up, they are generally safe and nutritious.
Diagnosis involves ruling out celiac disease first through blood tests while you are still eating gluten. If you need professional guidance on joint health, you can contact us for a consultation.
Yes. Besides dietary changes, patients often find relief through medical interventions. You can see our joint injection options or read about offloading knee braces for mechanical support.
The Dietary Guidelines for Americans recommend limiting added sugar to less than 10% of your daily calories to help manage overall health and inflammation.
No. A 2019 systematic review found no consistent evidence linking dairy consumption to increased inflammation in healthy adults.
NCGS is a condition where individuals experience symptoms like joint pain and brain fog after eating gluten, despite not having celiac disease or a wheat allergy.
Omega-3 fatty acids, found in fish and flaxseeds, can reduce the production of inflammatory cytokines that contribute to joint pain.
It is not recommended. You should consult a primary care provider or registered dietitian before starting an elimination diet, especially to ensure proper testing for conditions like celiac disease
While the typical Western diet is 15:1, a ratio of 4:1 or lower is considered more anti-inflammatory and better for managing joint pain.
Harvard T.H. Chan – Mediterranean Diet
At Joint Health Solutions, we combine evidence-based medicine with compassionate, patient-centered care. Our goal is to help you understand your joint pain, explore minimally invasive treatment options, and regain an active, pain-free life. Every recommendation is backed by peer-reviewed research and tailored to your unique needs.
Subscribe for wellness tips, treatment updates, and clinic news.
Trusted Expertise
Safe & Effective Care
Built Around You
Local & Accessible
© 2026 Joint Health solutions. All rights reserved.
Discover the innovative features of our software that streamline your workflow and enhance productivity. With user-friendly interfaces and powerful tools, you can easily manage tasks and collaborate with your team effectively.
© 2025 Joint Health solutions. All rights reserved.