Preparing for a shoulder injection? Ask these 5 key questions to understand the type, benefits, risks, and what to expect during recovery. Knowing the right shoulder injection questions to ask your doctor can make all the difference in your treatment outcome.
Shoulder pain from arthritis, impingement, or rotator cuff issues can be debilitating. When conservative treatments like physical therapy and oral medications aren’t enough, your doctor may recommend an injection.
But not all injections are the same. Cortisone, hyaluronic acid (HA), and PRP (platelet‑rich plasma) work differently, have different timelines, and carry different risks. Asking the right shoulder injection questions to ask before your procedure ensures you make an informed decision. In this article, we’ll cover the top 5 shoulder injection questions to ask your provider, plus additional considerations to help you feel confident and prepared.
When conservative treatments like physical therapy aren’t enough, shoulder pain treatment options including injections may be recommended.
Type | Mechanism | Best For |
Cortisone | Suppresses inflammation | Acute flare‑ups, severe pain, bursitis |
Hyaluronic Acid (HA) | Lubricates joint, reduces friction | Mild to moderate glenohumeral arthritis |
PRP | Uses concentrated platelets to stimulate healing | Chronic tendinopathy, partial rotator cuff tears, arthritis |
Ask your doctor:
– Why is this specific type best for my condition?
– Have you considered other options?
– What does the evidence say for my diagnosis?
Injection | Onset | Duration |
Cortisone | 1‑3 days | 4‑12 weeks |
Hyaluronic Acid (HA) | 2‑4 weeks | 6‑12 months |
PRP | 2‑6 weeks | 12‑24 months (if tissue heals) |
Ask your doctor:
– When can I expect to feel relief?
– How long will the effect typically last for someone like me?
– Will I need repeat injections?
Cortisone: Potential side effects increase with larger doses and frequent use. Risks can include cartilage damage, bone death, joint infection, nerve damage, tendon weakening or rupture, thinning of nearby bone or skin, and short-term flare of pain or increased blood sugar.
Hyaluronic Acid: Usually well tolerated, but may cause mild swelling, redness, or pain at the injection site and has a slight risk of infection or allergic reaction. Unlike cortisone, these injections provide longer relief and generally have fewer side effects, though repeated cortisone use can accelerate osteoarthritis progression.
PRP: A low‑risk procedure that uses your own blood. Less common risks include allergic reaction, bleeding, infection, nerve injuries, and tissue damage.
Ask your doctor:
– What are the most common side effects for this injection?
– How likely is a serious complication?
– How many of these injections have you performed?
Proper preparation improves safety and outcomes.
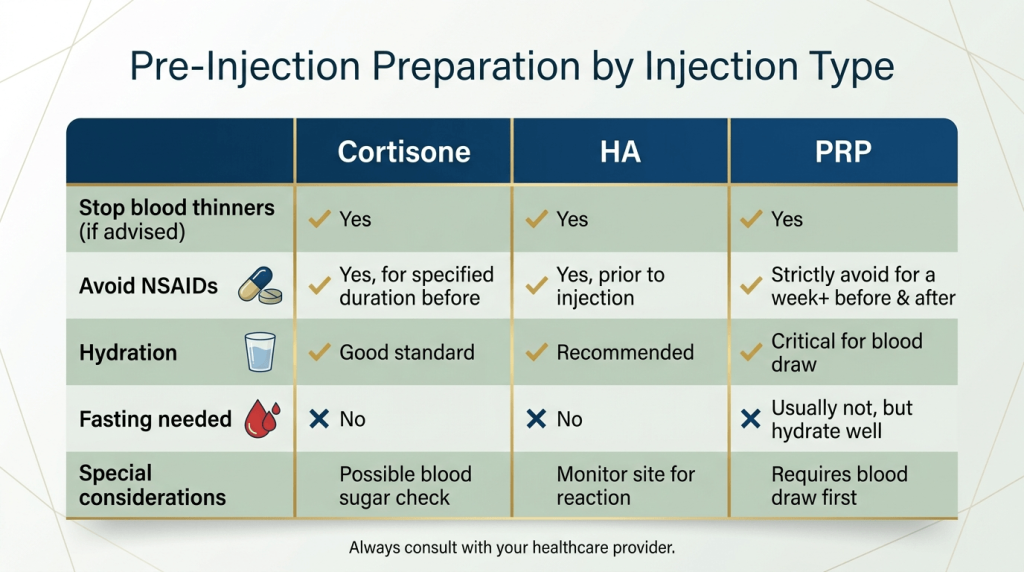
General preparation: Tell your doctor about all medications (especially blood thinners, insulin, NSAIDs) and report any allergies. You may need to stop blood thinners and supplements for a few days before the procedure. Arrange for a driver if sedation is planned and wear a loose‑fitting shirt or tank top.
For PRP specifically: Stop anti‑inflammatory medications (ibuprofen, naproxen, meloxicam) at least two weeks before the procedure and avoid corticosteroids for 4‑6 weeks. Hydrate well before the blood draw.
Ask your doctor:
– Should I stop any medications before the injection?
– Do I need to fast?
– Can I drive myself home?
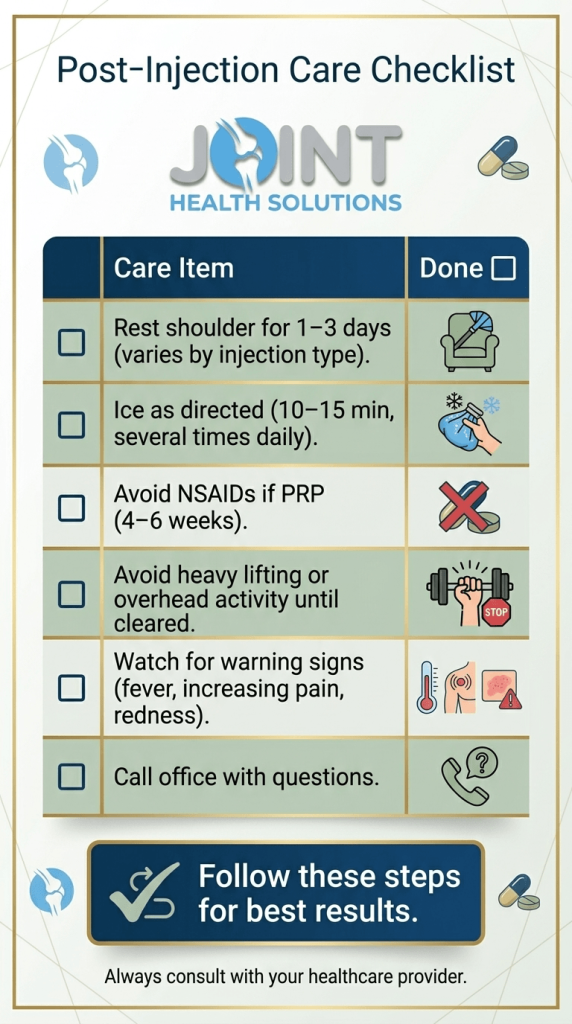
Cortisone: Protect the affected area for a day or two, avoid heavy lifting, and use ice on the injection site as needed. Don’t use heating pads or get in a hot tub for two days and watch for signs of infection. Monitor blood sugar if you have diabetes.
Hyaluronic Acid: Avoid heavy activity for 24‑48 hours; gentle range of motion is encouraged. Ice the area if sore.
PRP: Stay hydrated and eat nourishing meals. Don’t bathe, swim or use a hot tub for 48 hours. Avoid anti‑inflammatory medications for at least two weeks, minimize activity and ice the area for the first few days, and avoid strenuous activity for two weeks.
Expect some soreness – this is a normal healing response.
Ask your doctor:
– When can I return to normal activities?
– What activities should I avoid and for how long?
– What warning signs should prompt a call to the office? (e.g., increasing pain, fever, redness)

Beyond the top 5, here are more questions to ask:
– Will you use imaging guidance (ultrasound or fluoroscopy)? – Guidance improves accuracy, especially for deep joints like the glenohumeral joint.
– How many of these injections have you performed? – Experience matters.
– What is the success rate for my specific condition? – Realistic expectations are important.
– Can I have this injection if I’m also getting physical therapy? – Often yes, and they complement each other.
– How much will it cost? – Cortisone is usually covered; HA and PRP may have out‑of‑pocket costs.
– How many injections can I have over time? – Cortisone is limited (2‑3 per year per joint); HA and PRP can be repeated.
The right shoulder injection depends on your diagnosis, prior treatments, activity level, and goals. At Joint Health Solutions, we perform a thorough history and physical exam, review imaging (X‑ray, MRI, or ultrasound), discuss all options – including non‑injection alternatives – and perform injections under ultrasound guidance for precision. We provide clear pre‑ and post‑procedure instructions so you feel confident and informed.
Learn more about Shoulder Injections in Charlotte
Explore Cortisone Injections and PRP Therapy
Read our Patient Resources for more guidance
Most patients feel a brief pinch from the local anesthetic. The injection itself is usually well tolerated.
Cortisone: 1‑2 days. HA: 1‑2 days. PRP: 3‑7 days of relative rest (no heavy lifting or overhead activity).
Yes, unless sedation is used (rare). Most patients drive themselves.
Cortisone provides temporary relief. HA and PRP can offer longer‑lasting improvement by addressing lubrication or healing, but they are not always cures.
Cortisone: typically 2‑3 per joint per year. HA: as needed, often every 6‑12 months. PRP: 1‑3 initial series, then as needed.
Wait at least 4‑6 weeks after cortisone before PRP to avoid interference with healing.
For glenohumeral (ball‑and‑socket) joint injections, ultrasound improves accuracy significantly. For subacromial bursa injections, landmark guidance may suffice, but ultrasound is still helpful.
Cortisone is almost always covered. HA and PRP may not be covered; we’ll verify benefits beforehand.
Sometimes a different type or a repeat injection is needed. We’ll reassess and adjust the plan.
Call our office or book online. We’ll evaluate your shoulder and recommend the best approach.
American Academy of Orthopaedic Surgeons – Corticosteroid Injections for Shoulder Pain.
🔗 orthoinfo.aaos.org/en/treatment/corticosteroid-injections
Mayo Clinic – Shoulder injection: What you can expect.
🔗 www.mayoclinic.org/tests-procedures/shoulder-injection/about/pac-20394556
Hospital for Special Surgery – PRP for Shoulder Injuries.
🔗 www.hss.edu/condition-list_prp-shoulder.asp
Arthritis Foundation – Viscosupplementation for Shoulder Arthritis.
🔗 www.arthritis.org/health-wellness/treatment/treatment-plan/drugs/viscosupplementation
Discover the innovative features of our software that streamline your workflow and enhance productivity. With user-friendly interfaces and powerful tools, you can easily manage tasks and collaborate with your team effectively.
Subscribe for wellness tips, treatment updates, and clinic news.
Trusted Expertise
Safe & Effective Care
Built Around You
Local & Accessible
© 2025 Joint Health solutions. All rights reserved.
Discover the innovative features of our software that streamline your workflow and enhance productivity. With user-friendly interfaces and powerful tools, you can easily manage tasks and collaborate with your team effectively.
© 2025 Joint Health solutions. All rights reserved.