When it comes to joint injections, accuracy matters. Placing a needle into a small, deep joint—like the hip, facet joint, or sacroiliac joint—can be challenging without imaging guidance. Even for larger joints like the knee or shoulder, precise placement ensures that medication or regenerative material reaches the intended target.
Fluoroscopy-guided injections use real-time X-ray imaging to guide the needle to the exact location. This technology dramatically improves accuracy, safety, and outcomes.
At Joint Health Solutions, we use fluoroscopy for a wide range of injections, from cortisone and hyaluronic acid to PRP and trigger point injections. If you’re exploring treatment options, learn more about our joint injections.
In this article, we’ll explain how fluoroscopy works, why it’s superior to “blind” injections, and what conditions we treat with this precision technique.
Fluoroscopy is a type of medical imaging that displays a continuous, real-time X-ray image on a monitor. Think of it as an “X-ray movie” rather than a single snapshot.
During a fluoroscopy-guided injection:
This technology is widely used in orthopedics, pain management, and interventional radiology.
Inaccurate needle placement can lead to:
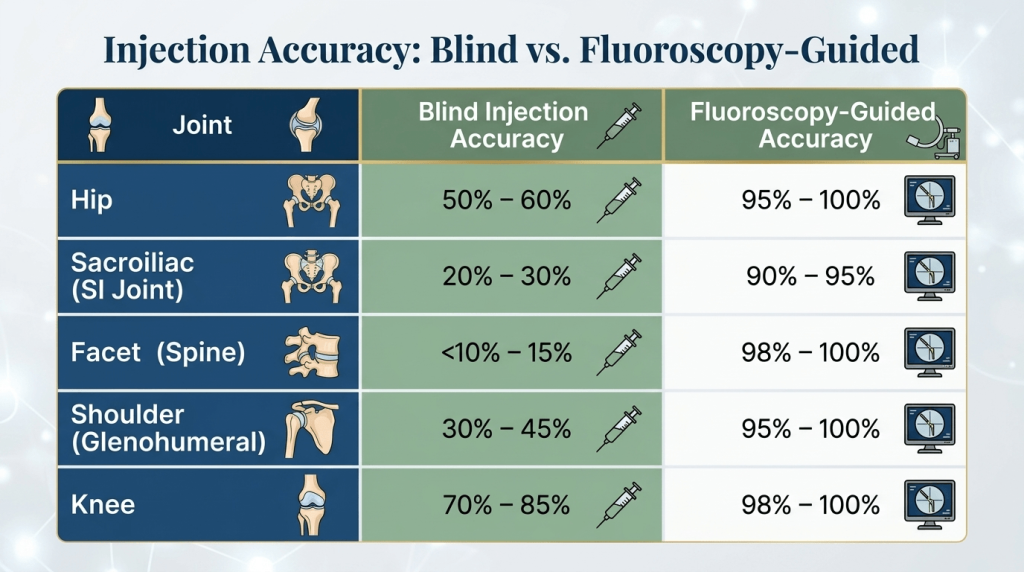
Studies show that “blind” (landmark-guided) injections miss the intended target up to 30-40% of the time in certain joints (e.g., hip, sacroiliac, facet joints). Fluoroscopy reduces this error rate to less than 5%.
For patients considering treatments like knee injections in Charlotte, precision plays a critical role in achieving optimal results.
We use fluoroscopy guidance for:
For standard knee or subacromial shoulder injections, we may use ultrasound guidance instead, depending on the anatomy and provider preference. You can also explore our shoulder injections in Charlotte for more common cases.
Benefit | Fluoroscopy-Guided | Blind |
Accuracy | >95% | 60-80% (varies by joint) |
Real-time visualization | Yes | No |
Ability to confirm spread | With contrast dye | Not possible |
Lower repeat injection rate | Yes | No |
Safety (avoids nerves/vessels) | Superior | Moderate |
Procedure time | Slightly longer | Shorter |
Radiation exposure | Minimal (low dose) | None |
For complex or deep joints, the benefits of fluoroscopy far outweigh the small radiation exposure and slightly longer procedure time.
Patients who have had limited success with traditional approaches may benefit from image-guided joint injections for improved accuracy and outcomes.
The entire procedure typically takes 10-20 minutes.

Fluoroscopy uses X-rays, which involve ionizing radiation. However, the dose used for a single injection is very low—comparable to a few chest X-rays or a dental panoramic X-ray. The benefits of accurate placement far outweigh the minimal risks.
We follow the ALARA principle (As Low As Reasonably Achievable) to minimize exposure:
Pregnant women should avoid fluoroscopy unless absolutely necessary.
Fluoroscopy guidance is especially valuable for:
For conditions like knee arthritis or shoulder impingement, we often use ultrasound guidance instead of fluoroscopy, as it offers real-time soft tissue visualization without radiation. Learn more about targeted options like knee injections and shoulder injections.
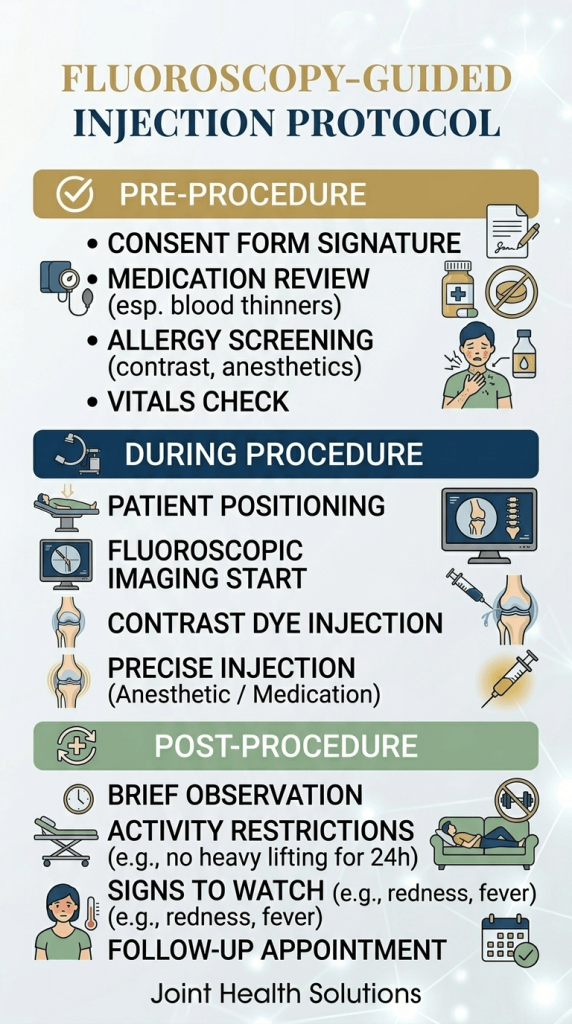
At Joint Health Solutions, we recommend fluoroscopy guidance for deep joint injections because it ensures precise needle placement. Unlike blind injections, fluoroscopy guidance provides real-time X-ray imaging, reducing error rates to less than 5%. Whether you need a hip, spine, or sacroiliac joint injection, choosing fluoroscopy guidance means better outcomes, fewer repeat procedures, and enhanced safety. If you’re seeking fluoroscopy guidance in Charlotte, our team is here to help.
Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec ullamcorper mattis, pulvinar dapibus leo.
Very low. A typical fluoroscopy‑guided joint injection delivers about 0.5‑2 mSv of radiation, equivalent to a few months of natural background radiation.
Generally avoided unless absolutely necessary. If you’re pregnant or might be, tell your provider.
Yes, unless sedation is used. If you receive sedation, you’ll need to fast for 4‑6 hours.
Typically 10‑20 minutes, plus a short observation period afterward.
Most patients do not require sedation. For very anxious patients or complex spine procedures, conscious sedation may be offered.
If cortisone is used, relief often begins within 24‑72 hours. If PRP or hyaluronic acid, it may take 2‑4 weeks.
Risks include infection, bleeding, nerve damage, or allergic reaction (very rare). Fluoroscopy adds no additional risks beyond those of any injection.
Yes, most insurance plans cover fluoroscopy‑guided injections when medically necessary.
Call Joint Health Solutions at 704-833-3566 to schedule your consultation.
Radiological Society of North America (RSNA) – Fluoroscopy.
🔗 www.radiologyinfo.org/en/info/fluoroscopy
American Academy of Orthopaedic Surgeons – Image‑Guided Injections.
🔗 orthoinfo.aaos.org/en/treatment/image-guided-injections
Pain Physician Journal – Accuracy of fluoroscopic vs. landmark‑guided injections.
🔗 www.painphysicianjournal.com/current/pdf?article=Mjg3MA%3D%3D&journal=88
Mayo Clinic – Fluoroscopy‑guided injections for joint pain.
🔗 www.mayoclinic.org/tests-procedures/fluoroscopy/about/pac-20394657
Discover the innovative features of our software that streamline your workflow and enhance productivity. With user-friendly interfaces and powerful tools, you can easily manage tasks and collaborate with your team effectively.
Subscribe for wellness tips, treatment updates, and clinic news.
Trusted Expertise
Safe & Effective Care
Built Around You
Local & Accessible
© 2025 Joint Health solutions. All rights reserved.
Discover the innovative features of our software that streamline your workflow and enhance productivity. With user-friendly interfaces and powerful tools, you can easily manage tasks and collaborate with your team effectively.
© 2025 Joint Health solutions. All rights reserved.